New York, NY – A critical care nurse at Stony Brook University Hospital in Suffolk County says that she and her exhausted colleagues expect to be “slammed” with new COVID-19 patients immediately after the state begins to reemerge from lockdown in May or June.
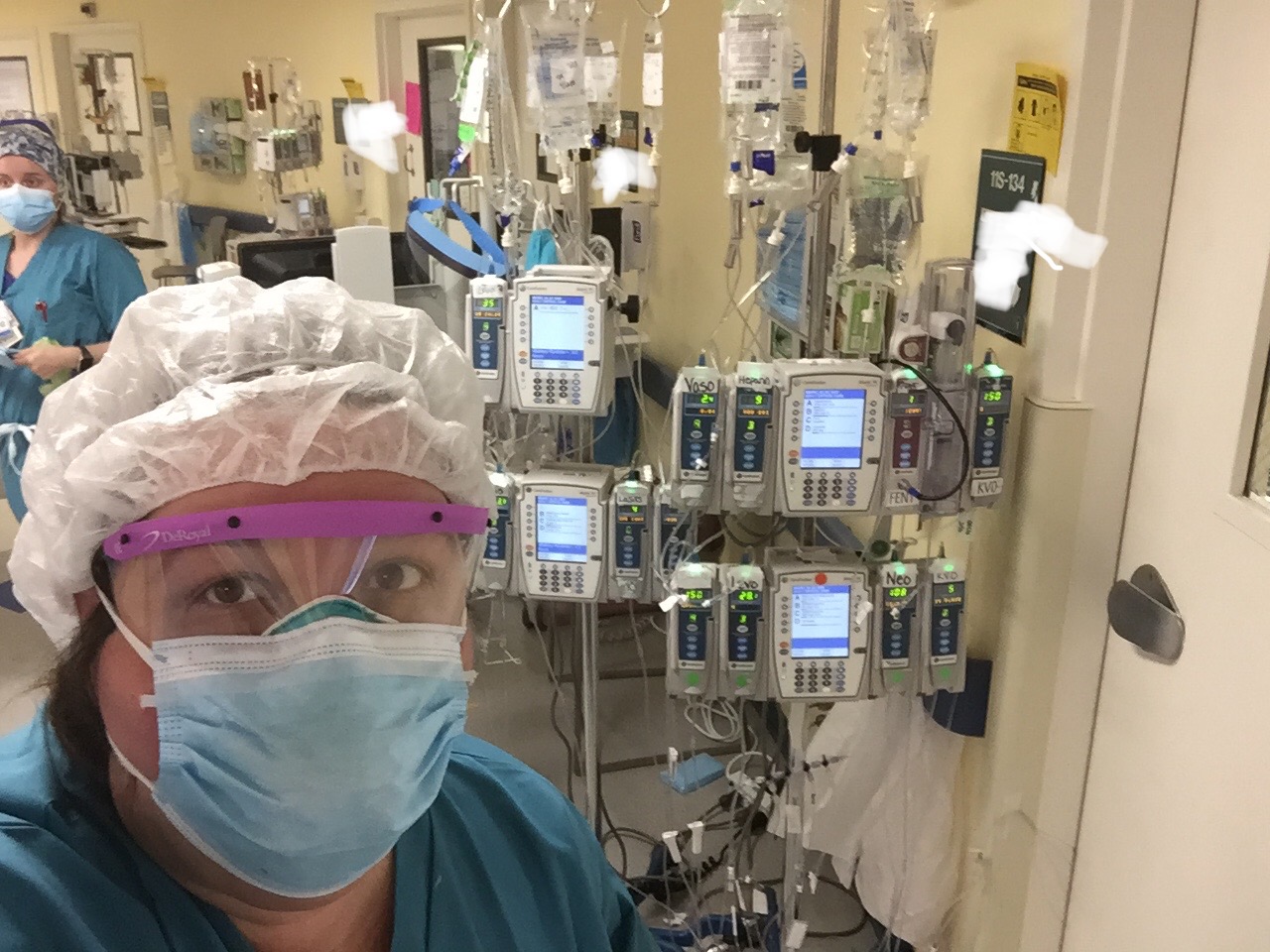
PEF member Amy Pacholk, 41, closes her eyes and can’t help seeing the ghastly, heartbreaking faces of her intubated patients fighting for their lives hooked up to the Level 1 trauma center’s ad hoc collection of indispensable ventilators.
Try as the might, Pocholk says the ICU remains full of COVID-19 patients who the staff simply cannot ween off the external breathing devices.
“I honestly can’t do this much longer; I don’t know how much more of this I can take,” the Green Port, Long Island mom recently told me.” I close my eyes and see my patients’ faces. If you ever saw what they look like — it is unbelievable. If you saw what it looked like, people would stay in their goddamned houses — I swear to god they would.”
Pacholk has been staying at a nearby hotel, too afraid of potentially exposing her asthmatic husband and cancer-surviving mom to the coronavirus. A number of Pacholk’s co-workers have been knocked out of action since the pandemic first began, but have since returned to work. Without adequate testing, Pacholk fears she might be asymptomatic and capable of spreading the virus.
Her eight-year-old daughter tries to be brave for her mom, but is beginning to show signs of depression and sadness. Social distancing kept mother and child apart during a recent, limited visit.
“‘It’s okay, mommy,” Pacholk’s daughter told her. “We’re here to help the corona — all of us.”
More than one million people across the United States and its territories have now tested positive for the COVID-19 coronavirus since the outbreak first began in Washington State on January 20. At the time of this writing, the nationwide death toll stands at 56,667—22,531 of those fatalities occurring right here in New York State — the epicenter of the COVID-19 pandemic in the U.S.
Absent negative pressure rooms — like the ones often associated with the treatment of Tuberculosis — everyone at Stony Brook’s ICU floors is “working dirty,” according to Pacholk. COVID-19 is everywhere.
“We could all be asymptomatic carriers — we’ve all been exposed in multiple ways,” she says. [Patients] are blowing air past their [breathing] tubes because the ventilators are set so high. Secretions are coming out of their mouths and noses. There’s just exposure everywhere.”
ICU patients typically require two- to three drips containing various treatments aimed at improving the “big picture” health for that particular person. Pacholk says COVID-19 patients sometimes need seven to twelve drips.
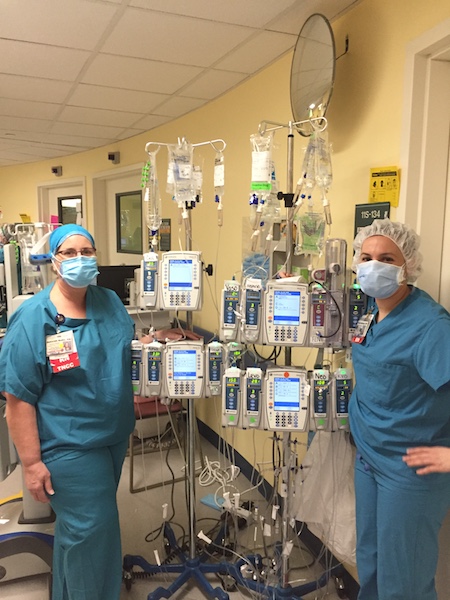
Hospital staffers darkly refer to these arrays as “Christmas trees.”
“It’s like a scary movie,” Pacholk says. “Those people are just not doing well and it’s unlikely that they’re going to make it.”
While the critical care specialists staffing Stony Brook’s ICU floors continue to have their hands full helping COVID-19 patients, new cases being admitted to the emergency have begun to drop off — and Pacholk attributes that to smart containment measures.
“There are still people coming in, but it’s not as bad as it was. And that’s probably because the social distancing seems to be working,” Pacholk says.
That can all easily change in a heartbeat, however. According to Pacholk, her hospital experienced an “uptick” in COVID-19 cases after Easter holiday celebrations.
“It was clear that there were some people getting together on Easter because our numbers did go up a little bit in one day,” Pacholk says.
Nevertheless, city and state officials across the country are beginning to make plans to restart their economies and end the lockdowns meant to contain the COVID-19 coronavirus.
Earlier this week, Texas Governor Greg Abbot, for example, unveiled plans to put the Lone Star State back in business by May 1.
New York City Public Advocate Jumaane Williams, last week, said that “ignorant arrogance mixed with entitlement” is “blowing up in our faces,” but that he doesn’t know what “the magic way” to reemerge from lockdown looks like.
Pacholk believes the pandemic is being politicized and that the welfare of working men and women is being dismissed.
“It’s said to say, but it seems to be the poorest people who are the sickest,” she says. “Initially, the people who we saw were white, they really were. Now, all the people we are seeing, they tend to be brown and black.“
The veteran healthcare professional and academic says that while some gravely ill patients have “shocked the business out of us” and gotten better, other patients who should have survived, have not.
“It’s mind boggling because these people are not fitting your prototype of what you’d would expect for people who would die,” Pacholk says.
Pacholk and her beleaguered colleagues working 15-hour days benefitted from the help of some 22 nurses from Syracuse and other areas around the state — without them, she says, the Stony Brook staff would not have been able to endure the onslaught of COVID-19 patients. And they’d be hard pressed to do it again.
The pandemic has demonstrated to Pacholk that systemic change elevating the rights of healthcare workers, is going to have to be implemented once this crisis is finally over. Either that, or the entire healthcare system itself will collapse.
“We are all just trying to work and do our job right now,” she says. “But I think when this is over, people are really fed up. I think we’ll get another hit in late summer, early fall. When it’s all over — maybe by next winter — I think you’re gonna actually see people quit. I think people are actually going to quit the healthcare world.”




2 thoughts on “Exhausted ICU Staffers Expect to Be ‘Slammed’ With New COVID-19 Patients After Lockdown Ends”
They are not going to make it? I have a family member in the covid unit and you’re announcing here that they are not going to make it. You should be ashamed of your bedside manner. I try to speak to a nurse and I am told no one is available so you just write an article and announce they won’t make it. Is this how Stony Brook hospital treats families now! Disgusting!!!!
Thank you for all you do . My brother in law was released today . He has been there since March 29th and was on a ventilator for about 11 days. You are the true hero’s